
Early Nutrition Intervention for Pediatric Health Equity
Challenge
Childhood Type 2 Diabetes is rising rapidly among underserved families due to limited access to fresh, affordable nutrition, increasing long-term health risks for children ages 5–12.
My Role
Owned this end-to-end, leading research, synthesis, and system-level solution design in collaboration with healthcare, nonprofit, and community stakeholders.
Predicted Outcomes
Modeled projections based on early-intervention and Food-as-Medicine literature.

$40–$80 savings/ month
120+ data points 60+ households
(single + two-parent)

10–20% reduction
in preventable nutrition-related risk factors
8 nonprofits (5 responses, 3 collaborators)
Retail partners (CVS, Kroger)

15–30% improvement
in Operational efficiency
SNAP/WIC-compatible
Nonprofit + retail integration (CVS, Kroger, 912 FF)
Cost of Type 2 Diabetes in the U.S.
$400B/ year
• 1 in 4 U.S. healthcare dollars goes toward diabetes care• $400B+ spent annually across treatment and management• One of the largest drivers of healthcare spendingType 2 Diabetes in the U.S. and Financial Costs

35%
of U.S. children are overweight or obeseProblem – Rising Type 2 Diabetes in U.S. Children

20%
increase in childhood Type 2 Diabetes over the past decade
Diabetes Costs in the U.S. – Impact on Families

5–40%
of household income out of pocket
Problem
Despite the urgency, families in underserved communities face structural barriers that make healthy nutrition inaccessible.
Common Challenges Households - Single parent and Two parent
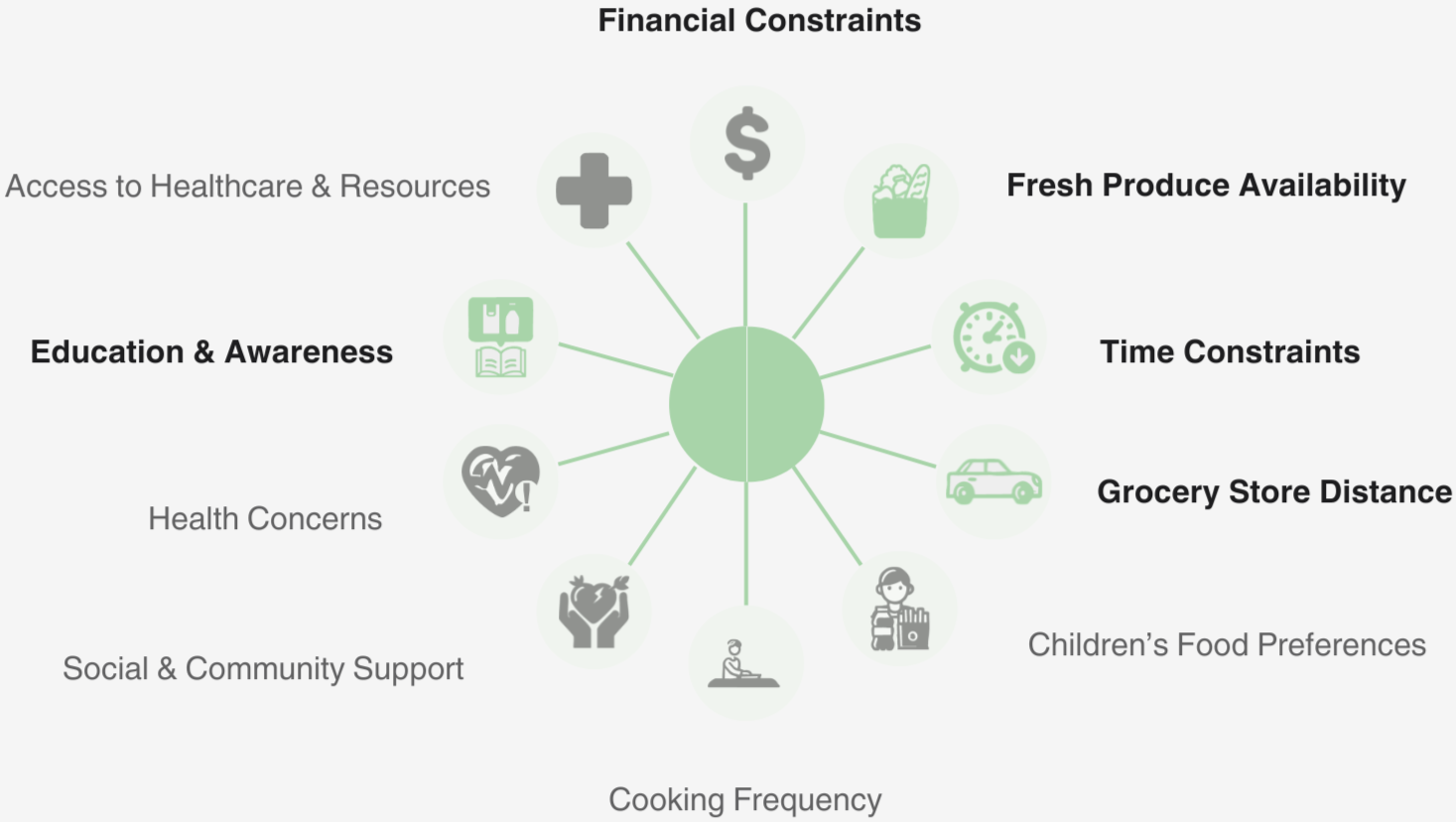
Key Barriers - Families

Fresh Produce is Costly

Limited Time

Distance from Fresh Produce
Opportunity
Early nutrition intervention presents a critical opportunity to prevent long-term health risks for children ages 5–12 by improving access, affordability, and guidance for underserved families.
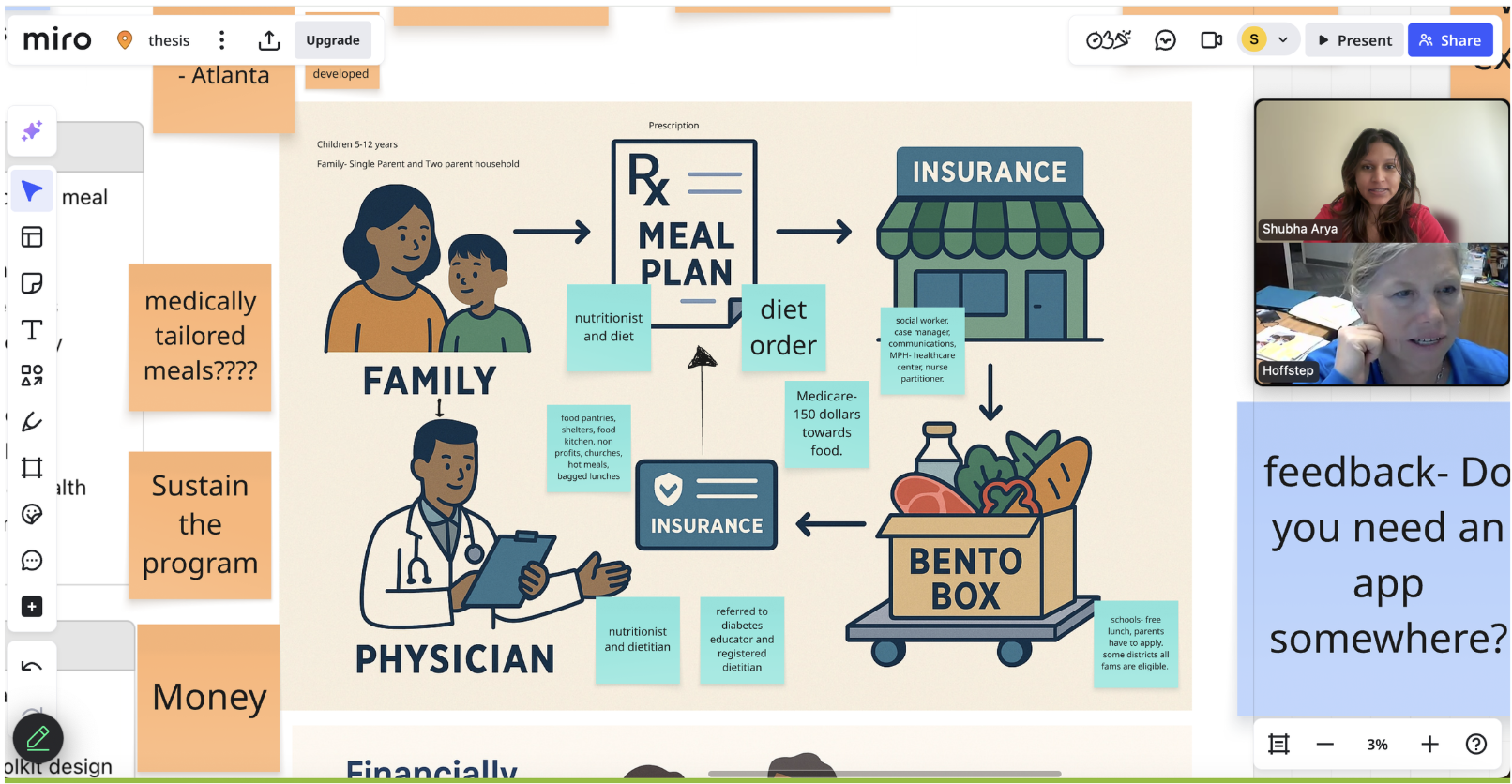
Proposed Solution

1. Family Context, children (5-12) years

2. Financial Barriers

3. Tailored Provider Guidance

4. Insurance-Covered, tailored Meal Plans

5. Produce Delivery

6. Fresh Produce Kits/ Insurance-Covered
Illustrations by Jayanti Dave, developed collaboratively from hand-drawn concept sketches.
Cost-Nutrition-Health Connection in At-Risk Children
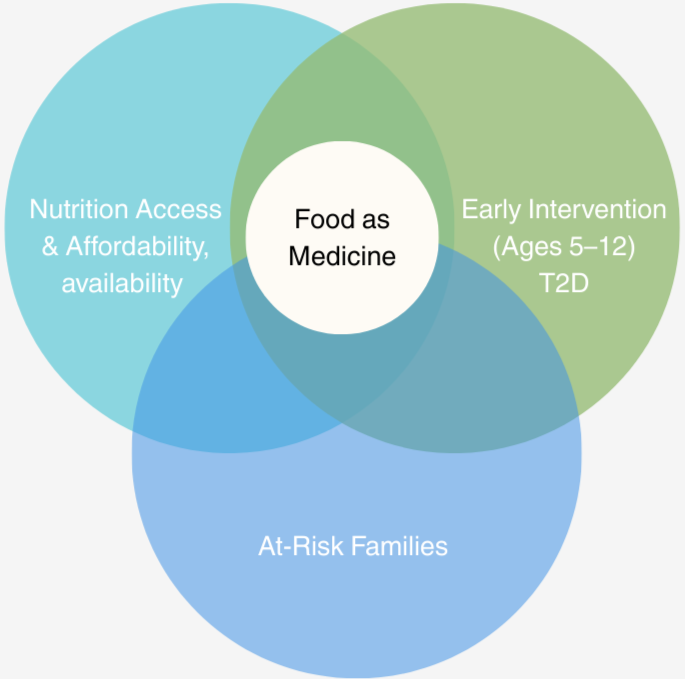
This overlap reveals a clear opportunity to leverage food-as-medicine as an early intervention pathway—bringing affordable, culturally relevant nutrition to at-risk children during the most critical years of preventing Type 2 Diabetes.
Research and Insight
Research across families, nonprofits, and healthcare providers revealed systemic gaps in access, affordability, and nutrition support contributing to pediatric Type 2 Diabetes.
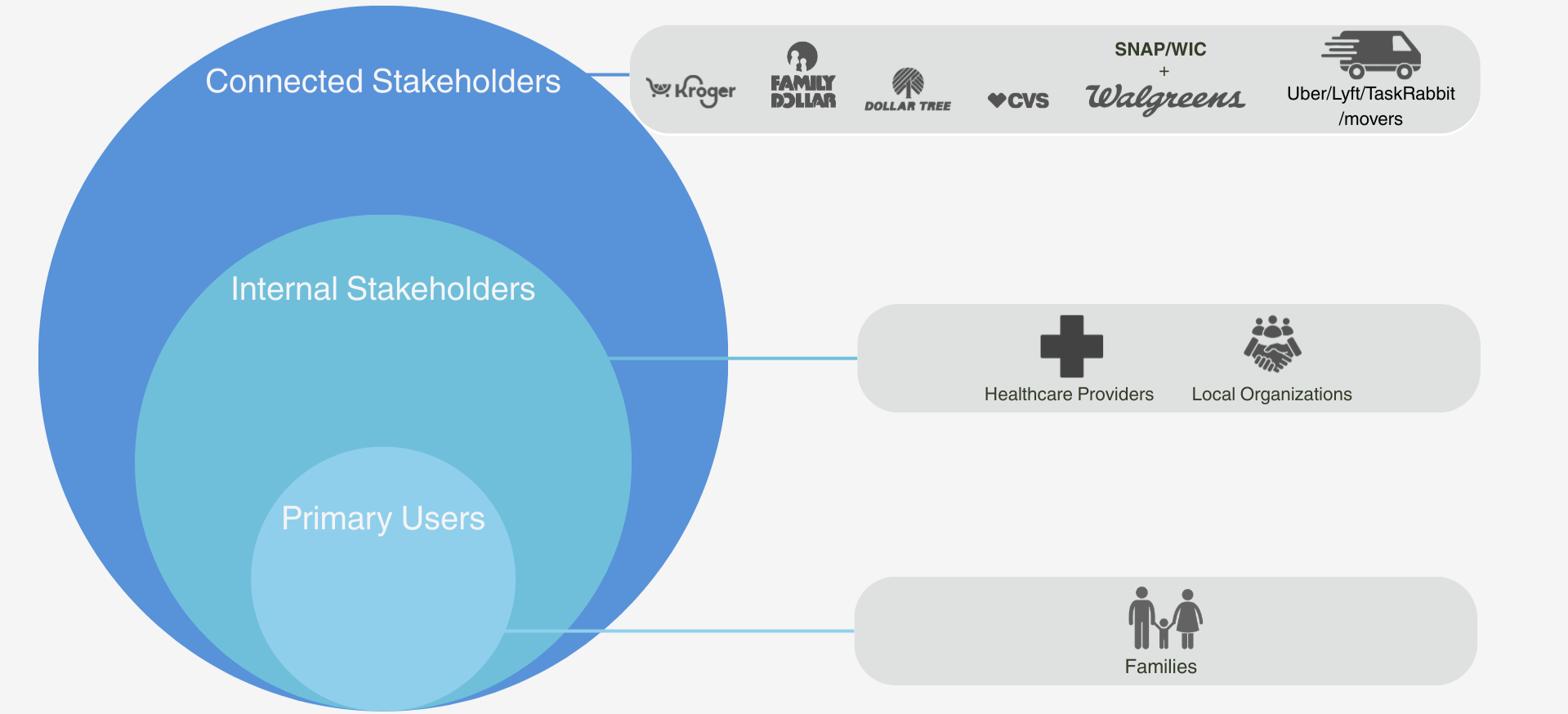
Key Players

Families
20- Two Parent
20 - Single Parent
130- Both Households

Local Organization
5- Nonprofits
7- Stakeholders

Healthcare Providers
3- Hospital
4- Clinics
9- Providers
Ecosystem Map
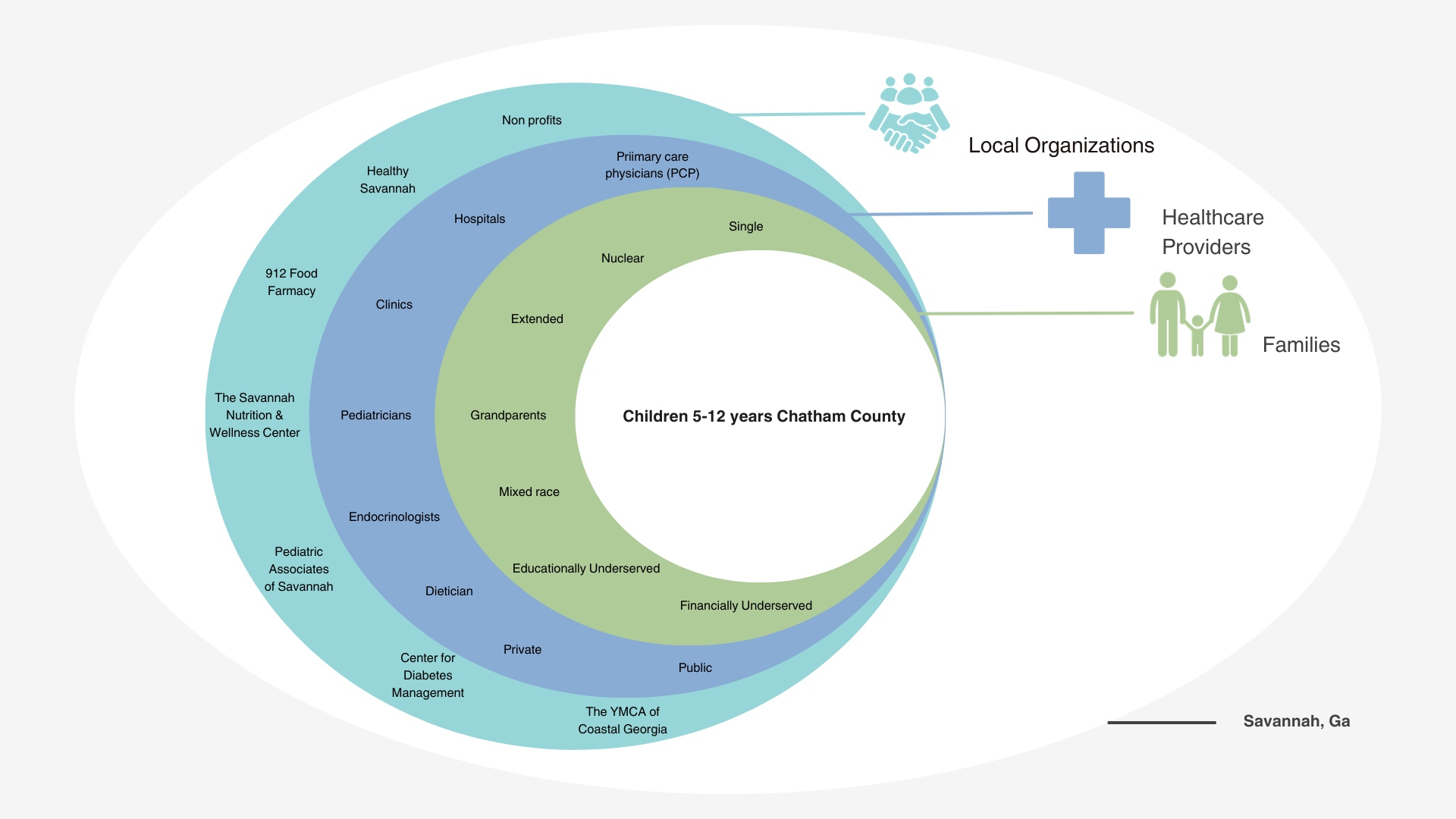
Current landscape - Savannah, Ga at the time of study
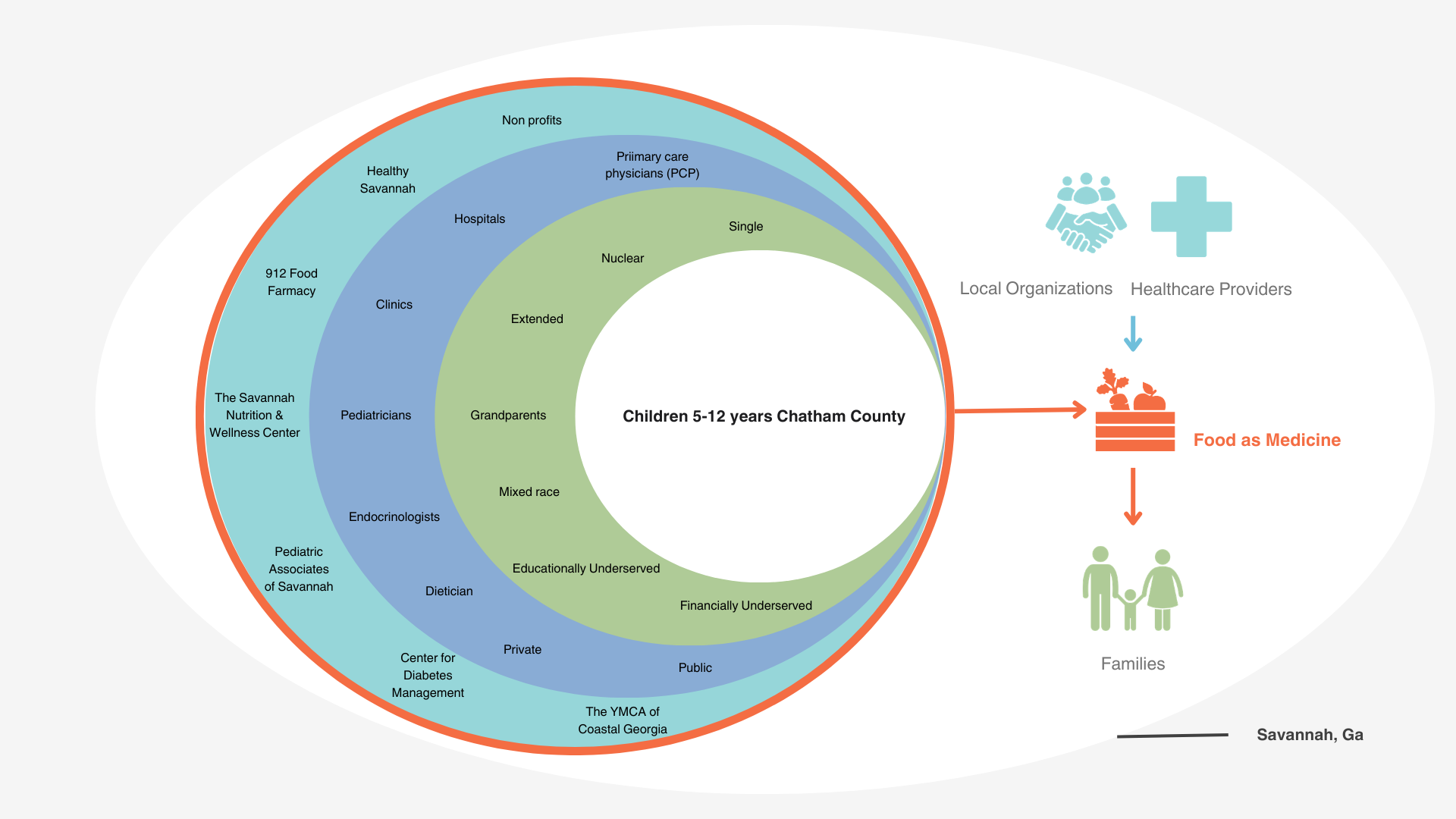
Post Intervention landscape - Savannah, Ga at the time of study
AI-Augmented Research & Synthesis
Sample Example
AI-supported quantitative and qualitative analysis using ATLAS.ti
Synthesized insights from 80+ peer-reviewed and mixed-method sources on childhood nutrition, food access, and Type 2 diabetes
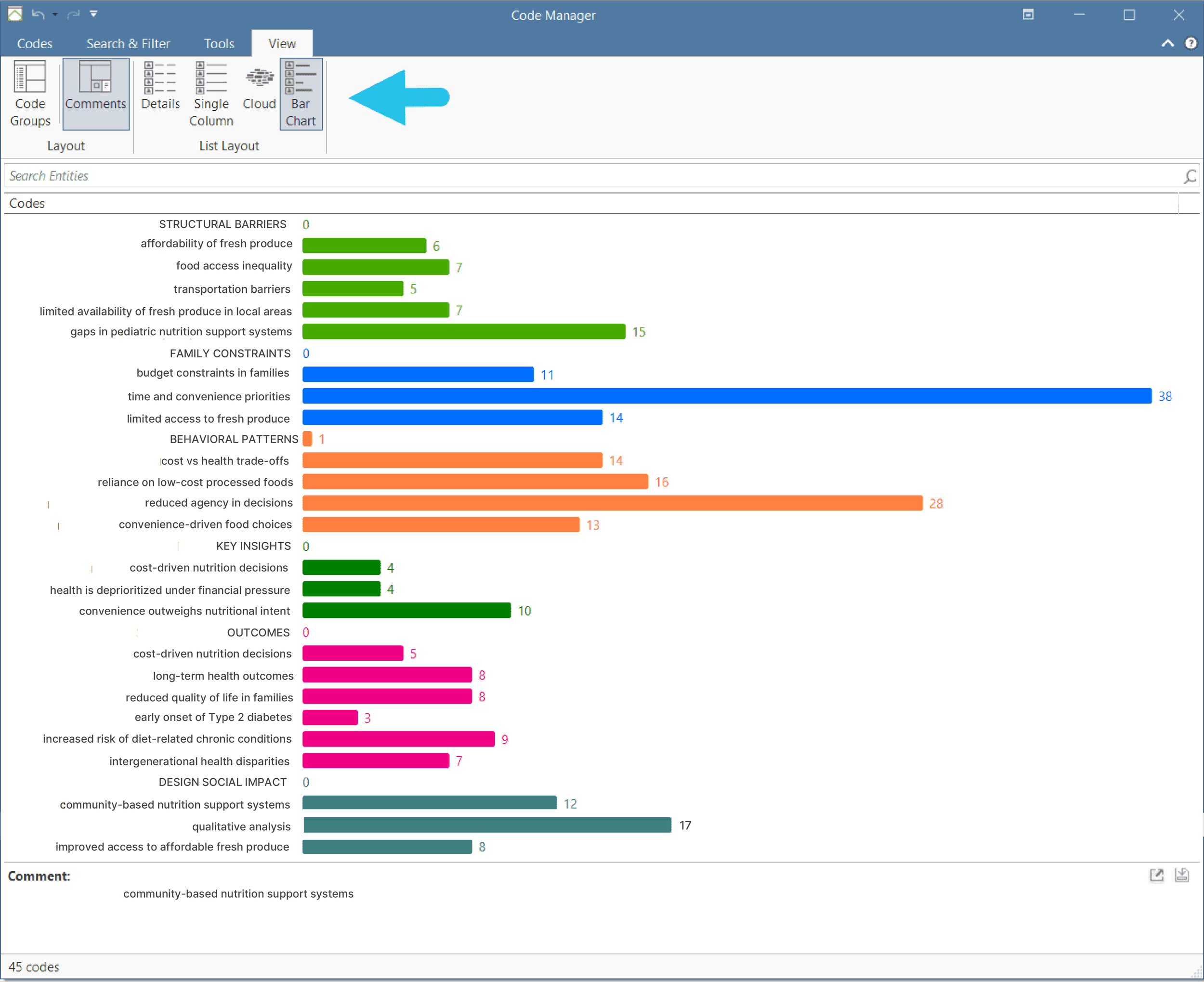
Analyzed 120+ survey responses and conducted in-depth interviews with 60+ families to understand real-world constraints, behaviors, and decision-making patterns
Validated concepts with 8 cross-sector stakeholders (public & private healthcare, nonprofit leadership, and food retail partners) through collaborative Miro workshops
Sample Example
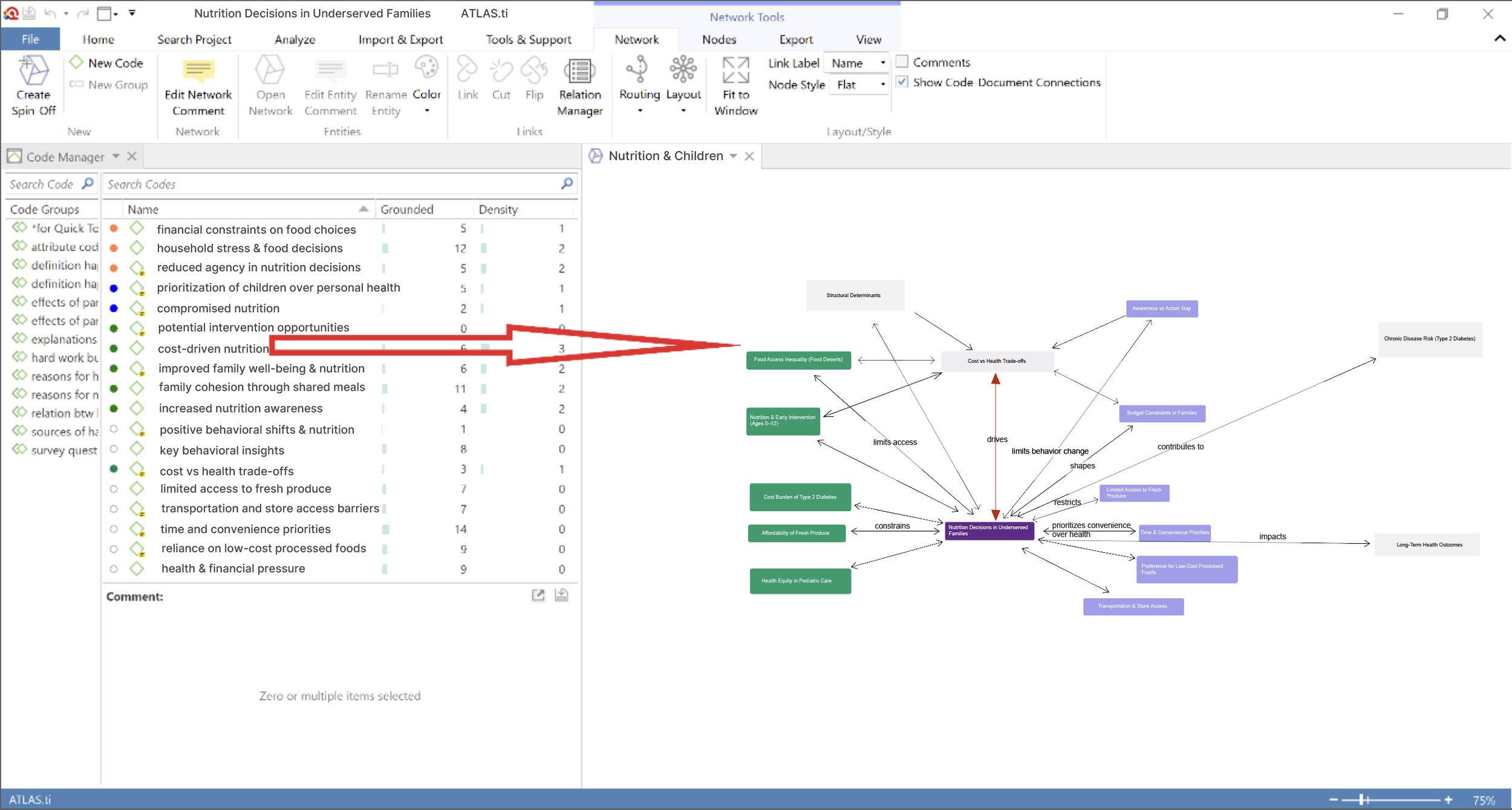
Concept Development 1 & 2









Synthesized stakeholder feedback collected via Miro co-creation sessions. Icons indicate participant type.
Key Players


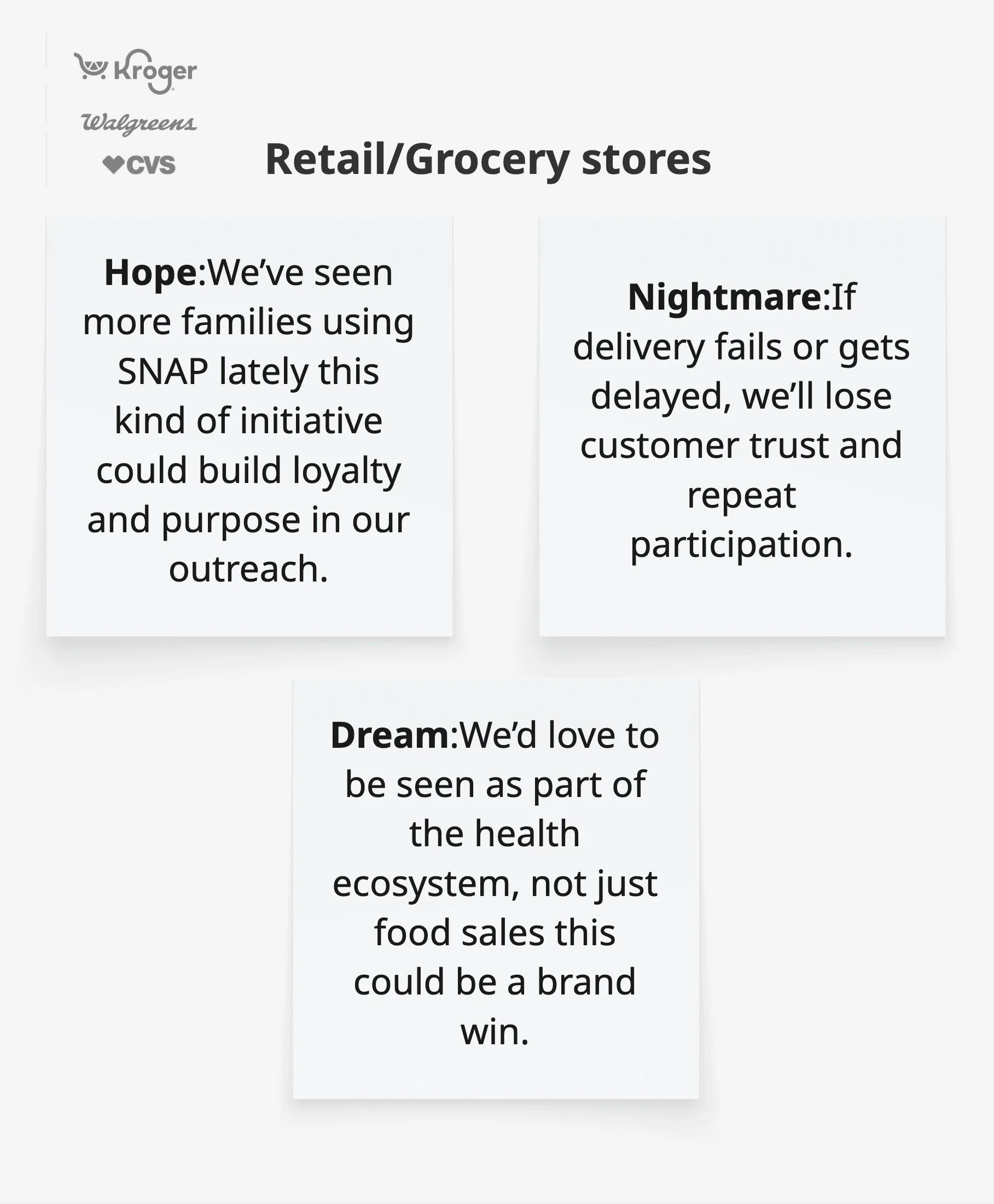
Families


Insight Consolidation: From Clusters to Key Takeaways
Sample Example

Design Approach
The process followed the Double Diamond framework, balancing research depth with iterative prototyping and validation (in full presentation).
Ethical Design
Ethical Design
Ensured equitable access, cultural sensitivity, and responsible use of data by prioritizing underserved families and minimizing barriers to participation.
Value Proposition
A culturally and clinically tailored fresh produce–kit service designed to improve nutrition access for financially underserved families in Savannah.
A culturally and clinically tailored fresh produce–kit service that improves nutrition access for underserved families by combining SNAP/WIC compatibility, physician-approved guidance, and local nonprofit and retail partnerships.
Value-Based Care
Aligned with Value-Based Care Models
Shifts focus from treatment to prevention, reducing long-term healthcare costs while improving outcomes for children and families.
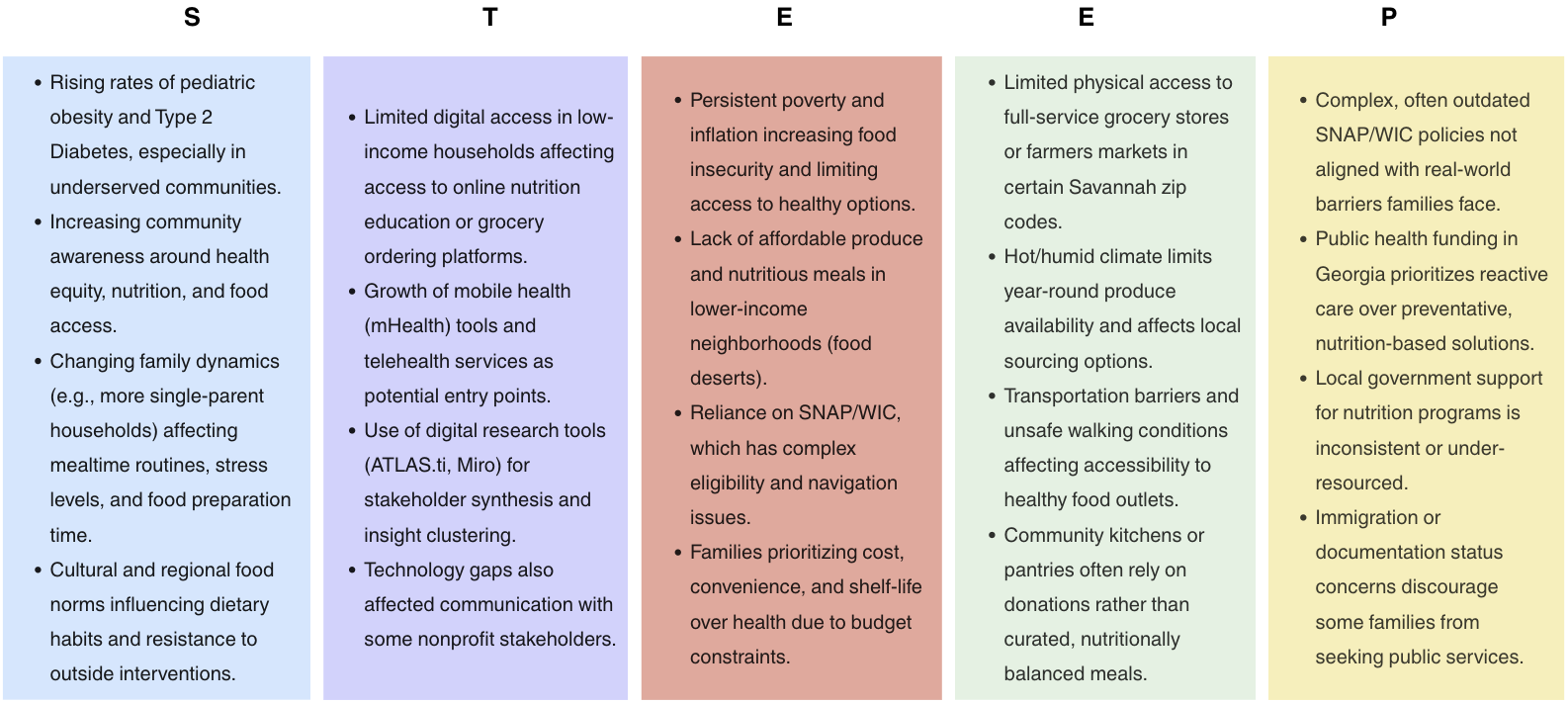
STEEP Factors - Impact on Study 2024-2025
STEEP was focused on Savannah, GA and my thesis study reducing type 2 diabetes in financial undeserved families and children.
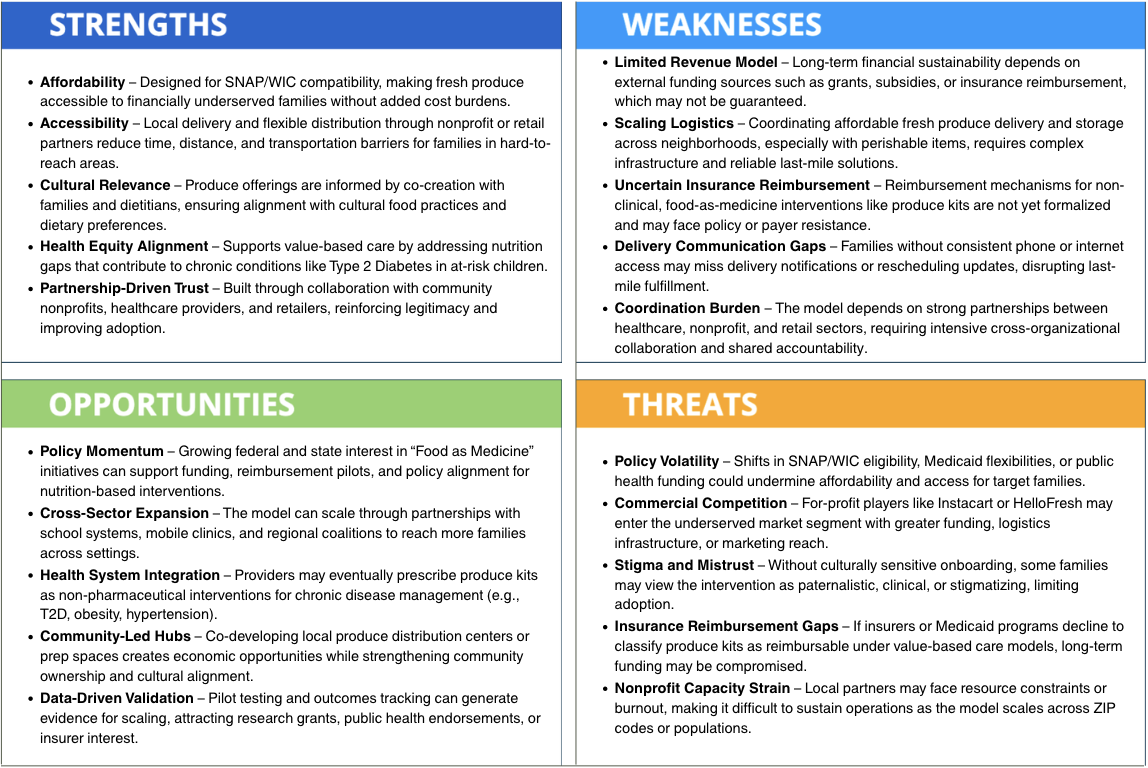
SWOT Analysis for Concept: The Food as Medicine Family Initiative
Competitive Benchmarking
Competitive Benchmarking - Takeaways
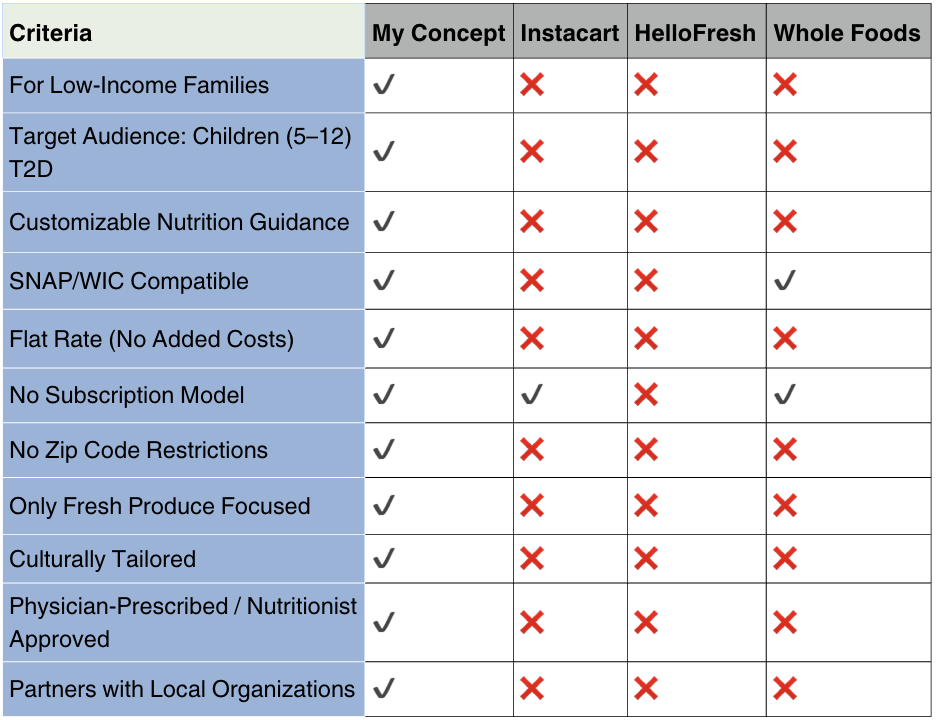
Bridges a Critical Gap
Built for the Underserved
Locally Rooted & Clinically Informed
More Than Delivery, It’s Directional
From Access to Alignment
Value of Concept

Customizable Nutrition Guidance

SNAP/WIC Compatible & Cost Transparent

Flat Fee

Built on Community Partnerships

Convenient

No Zip Code Limits

Fresh Produce Only
Pilot Session & Key Takeaway
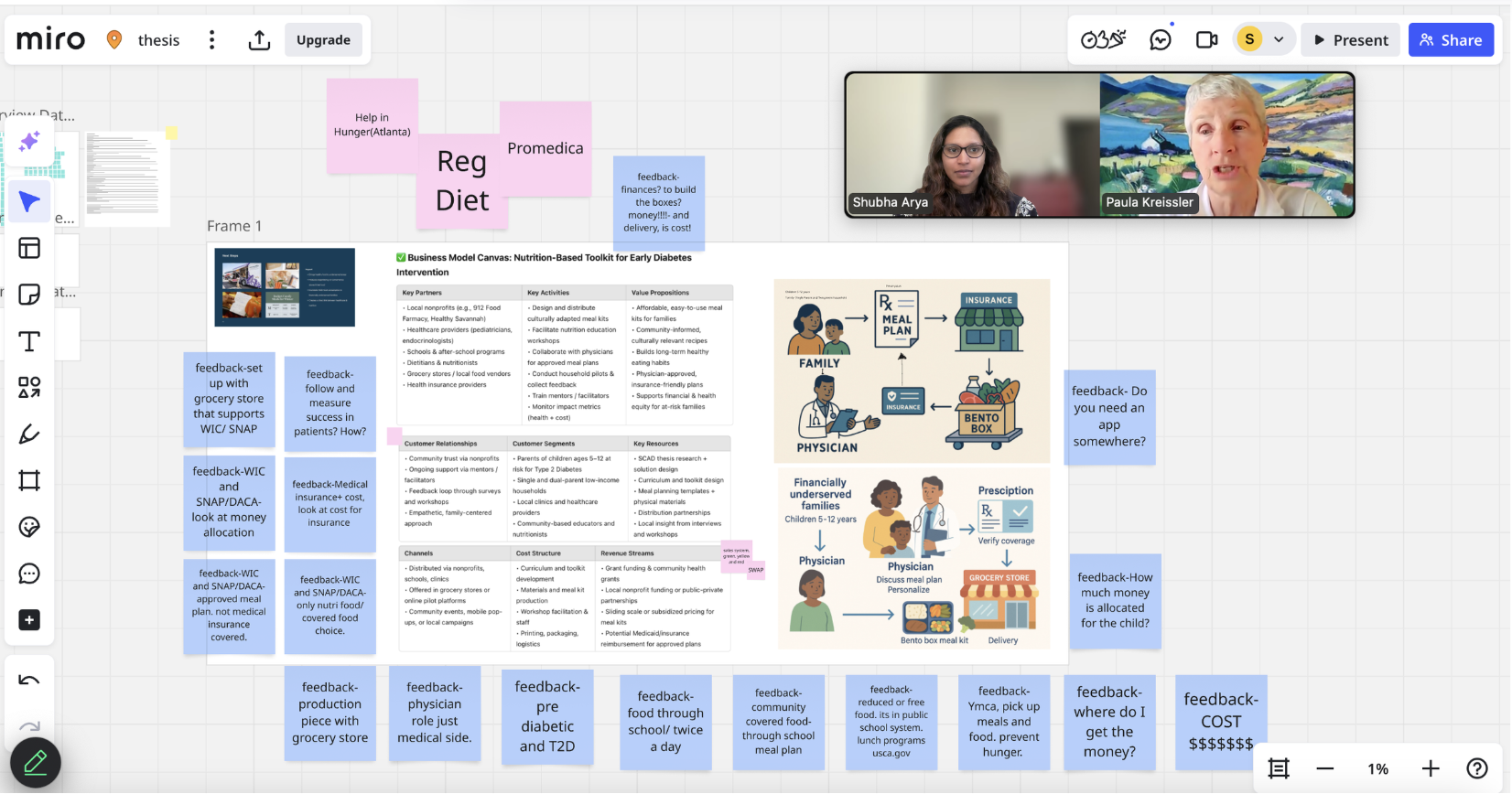
Funding is Limited For Nonprofits
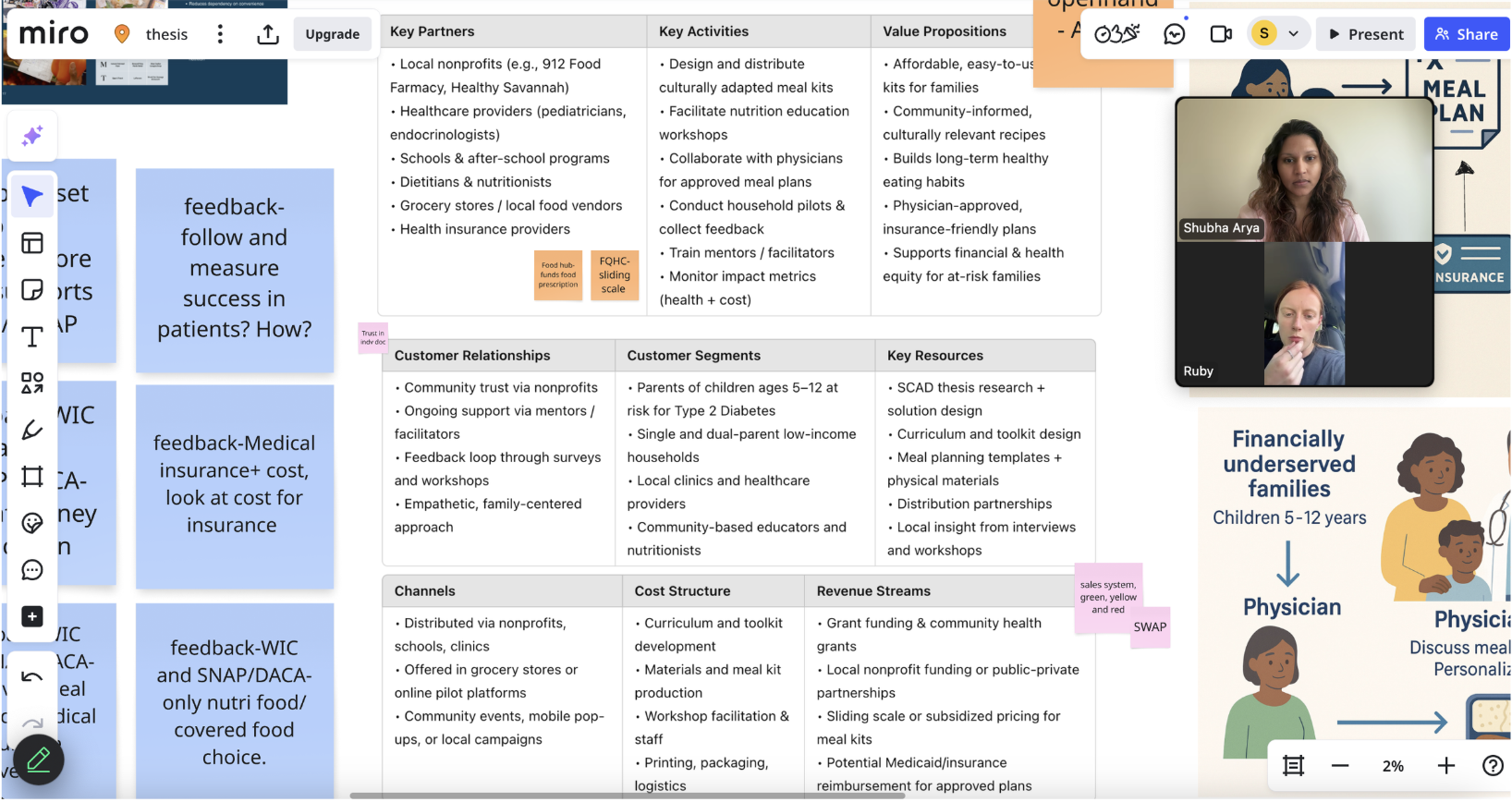
Leverage Existing Infrastructure
Insurance doesn’t Cover Food
Concept Validation
Learnings/Findings
Physician-aligned guidance delivered through trusted community partners increases adoption and credibility.
Non-subscription, SNAP/WIC-compatible models reduce cost, time, and access friction.
Leveraging existing nonprofit and retail infrastructure enables scalable implementation.
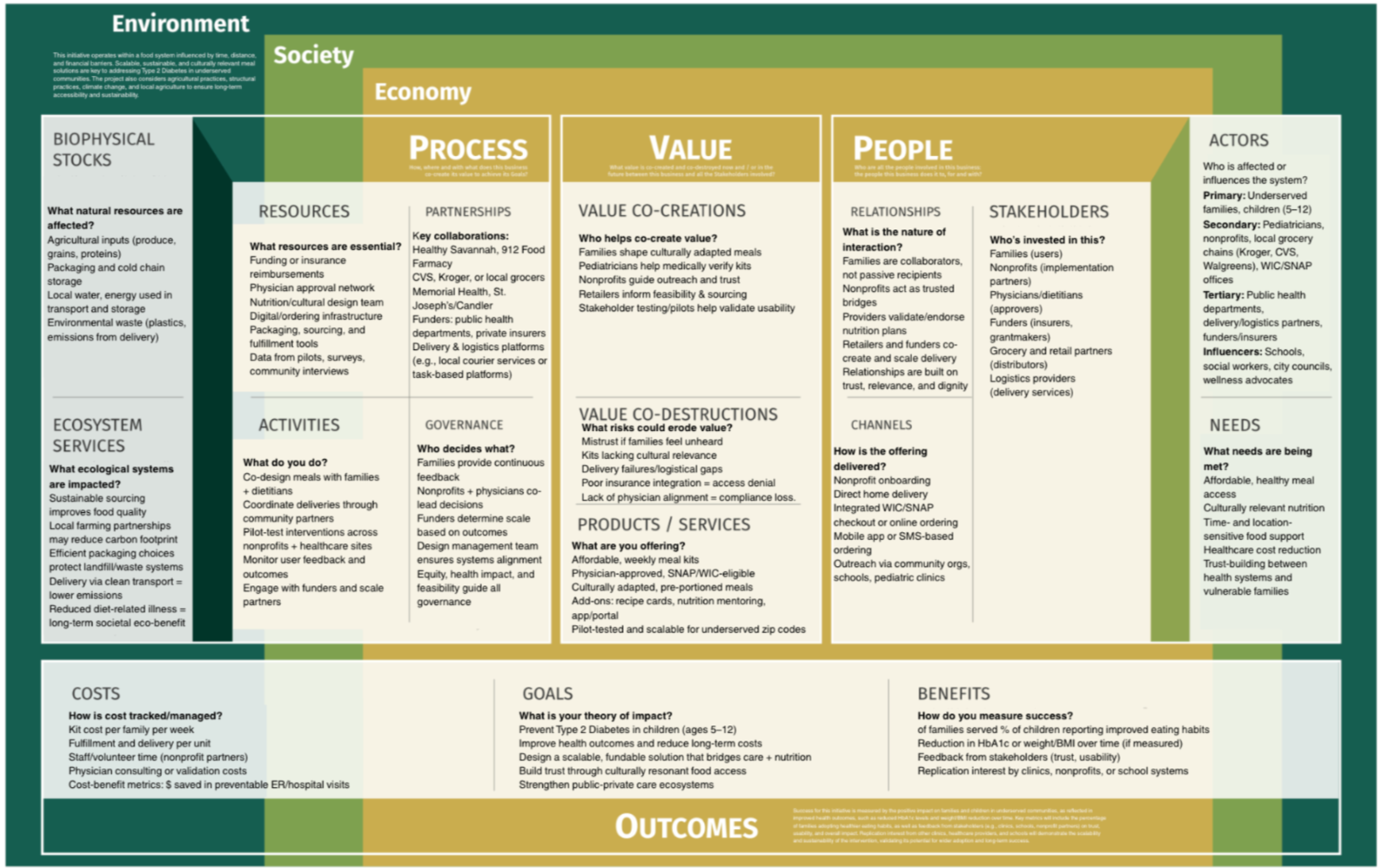
Flourishing Business Canvas(FBC)- Food as Medicine Family Initiative
Key Takeaways

Community Collaboration Supports Tailored Nutrition

All Stakeholders Play an Equal Role

Collaboration is Key
Next Steps

912 Food Farmacy (Non profit in Savannah, Ga


(A common grocery store franchise in Savannah, Ga)
=

Long-Term Sustainability
Process Development

Insight synthesis (ATLAS.ti + AI)
Concept iterations + selection logic
Translating insights into design decisions

Prototype + stakeholder validation